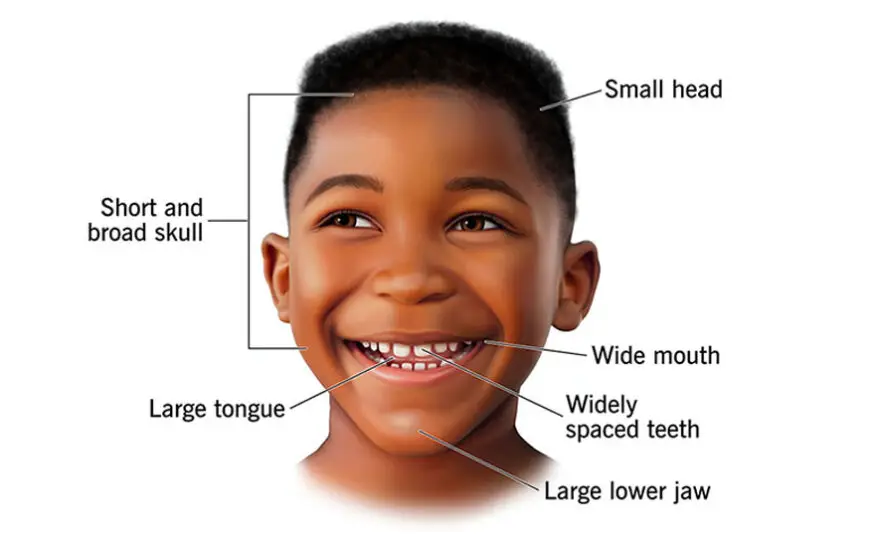
Angelman Syndrome is a rare neurogenetic disorder that affects neurological development, movement, communication, behaviour, and daily functioning. It occurs due to dysfunction of the UBEЗA gene located on Chromosome 15, which plays a crucial role in brain development and neural communication.
Children with Angelman Syndrome typically present with developmental delays, severe speech impairment, balance and coordination difficulties, seizures, sensory processing differences, and a characteristically happy and excitable demeanour. While there is no cure, early therapeutic intervention-especially occupational therapy-significantly improves functional independent participation in daily life.
This article focuses on the role of occupational therapy and therapeutic strategies that support development and quality of life. Understanding Functional Challenges.
Children with Angelman Syndrome often experience difficulties in: Sensory processing and regulation, Balance, coordination, and motor planning, Fine motor control and hand function, Feeding and oral-motor coordination, Attention and engagement, Self-care and daily living skills, Communication and social participation, Occupational therapy addresses these areas to enable meaningful participation in home, school, and community environments.
Importance of Early Intervention: Early therapy helps the developing brain build functional pathways and prevents secondary complications.
Intervention supports: Postural stability and motor control, Sensory modulation and attention, Independence in self-care, Functional communication, Participation in play and learning, A structured, individualized therapy plan produces the best outcomes.
Occupational Therapy: Core Areas of Intervention Occupational therapy (OT) aims to improve a child’s ability to perform daily activities independently and participate actively in life roles. Therapy is play-based, structured, and adapted to the child’s sensory and developmental needs.

- Sensory Processing and Regulation: Children with Angelman Syndrome often seek movement and deep pressure input, and may have difficulty regulating arousal levels and attention, Therapeutic Strategies, Vestibular Activities, Swinging and rocking, Gentle spinning activities, Balance board exercises, These improve balance, alertness, and spatial orientation, Proprioceptive Input, Pushing and pulling weighted objects, Climbing and crawling through tunnels, Carrying weighted toys or bags, These activities enhance body awareness and calming regulation, Deep Pressure Techniques Therapy ball pressure over limbs and back, Joint compressions (guided by therapist), Weighted blankets or lap pads, Deep pressure provides calming sensory input and improves attention, Tactile Play, Sand, rice, foam, clay, textured fabrics, Water plays and sensory bins, Tactile exposure improves sensory tolerance and exploration. A personalized sensory diet supports self-regulation throughout the day.
- Postural Control and Gross Motor Development: Children frequently exhibit ataxic gait, poor balance, and reduced core stability. OT Interventions, Therapy ball exercises for trunk control, sitting balance activities on dynamic surfaces, Obstacle courses to improve coordination, Stepping over objects and balance beam walking, Tricycle riding and trampoline jumping, Improved postural control enhances attention, hand function, and mobility.
- Fine Motor Skills and Hand Function: Fine motor delays affect play, feeding, and pre-academic readiness. Therapeutic Activities, Squeezing putty and soft balls to strengthen grasp, Bead threading and stacking rings, Pegboards and shape sorting, Scribbling, colouring, and early pre-writing strokes, Bilateral activities such as tearing paper or opening containers, Developing hand strength and coordination supports independence in daily tasks.
- Activities of Daily Living (ADL) Training: Occupational therapy promotes independence in self-care skills. Feeding Skills, Spoon use training and finger feeding practice, Improving lip closure and chewing skills, managing drooling and oral sensitivity, Introducing adaptive utensils when needed Dressing Skills, removing simple garments, Pulling pants up and down, Practising Velcro fasteners and large buttons, Grooming Skills, Tooth brushing with guided assistance, Face washing and hair grooming routines, Sorting shapes and colours, These skills support play participation and early learning readiness.
- Attention, Engagement, and Play Development: Short attention span and high excitability can affect participation. OT Strategies, Short, structured activity sessions, Cause-and-effect toys to promote engagement, Turn-taking games to build social interaction, Music and rhythm-based activities to improve focus, Visual schedules to provide predictability, Play-based therapy enhances motivation and supports cognitive development. Oral-Motor and Feeding Intervention, Oral-motor challenges may include tongue thrusting, drooling, and chewing difficulty. Interventions, Oral-motor stimulation exercises, Straw drinking and blowing bubbles, Chewing practice with safe textured foods, Lip closure and tongue mobility exercises, Improved oral control supports feeding and communication readiness.
- Adaptive Equipment and Environmental Modifications: Occupational therapists may recommend, Adaptive seating systems for posture and stability, Non-slip bowls and modified spoons, Weighted lap pads for calming and attention, Visual schedules and picture communication supports, Environmental adaptations promote independence and reduce frustration. Multidisciplinary Collaboration.
- Optimal outcomes require teamwork: Physiotherapy improves gait and mobility, Speech therapy develops communication and AAC use, Behavioural therapy improves attention and adaptive behaviour, medical care manages seizures and sleep issues, Special education provides structured learning support, Collaborative care ensures comprehensive development. Strength-Based Therapeutic Approach.
- Children with Angelman Syndrome demonstrate many strengths that can be used to enhance therapy: Strong social interest and affection, Joyful and engaging personality, Love for music and rhythmic movement, Positive response to visual learning, Enjoyment of sensory-rich activities, Using strengths increase motivation and participation. Conclusion, Angelman Syndrome presents lifelong developmental challenges, but occupational therapy plays a transformative role in promoting independence, sensory regulation, motor skills, and participation in daily activities. Through individualized intervention, sensory integration strategies, ADL training, and play-based therapy, children can develop functional skills that enhance their quality of life, Early intervention, caregiver involvement, and multidisciplinary collaboration are key to maximizing developmental outcomes. With appropriate therapeutic support, children with Angelman Syndrome can lead joyful, meaningful lives and actively participate in their families and communities.
Dr. Subhalaxmi Behera
Consultant Senior Occupational Therapist (Clinical)
Auticure Child Development Centre, BBSR